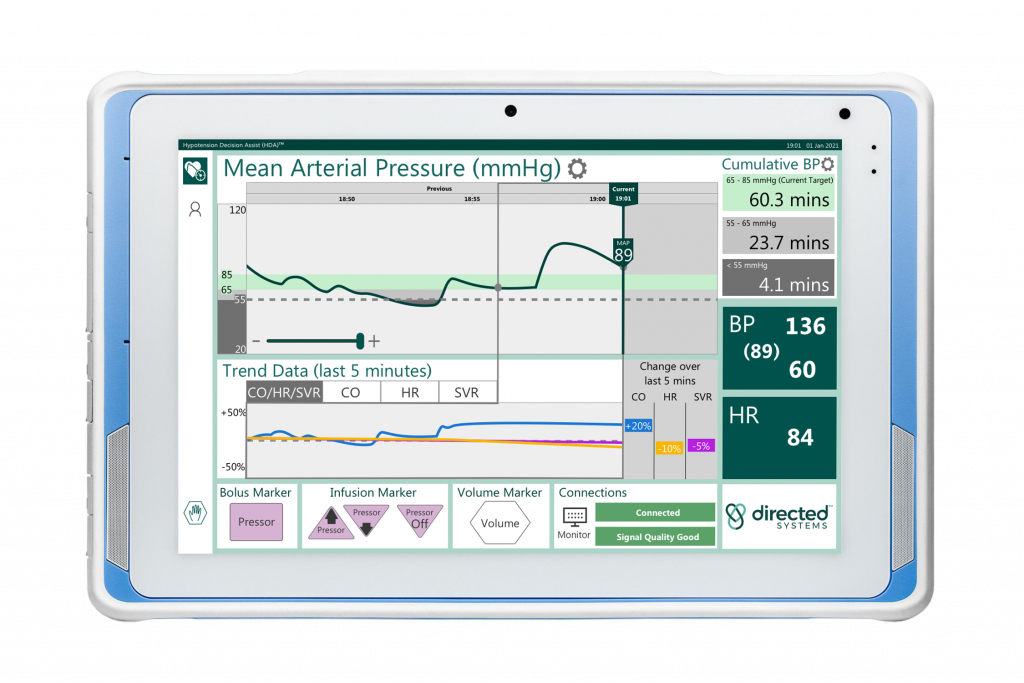
HDATM Main Screen
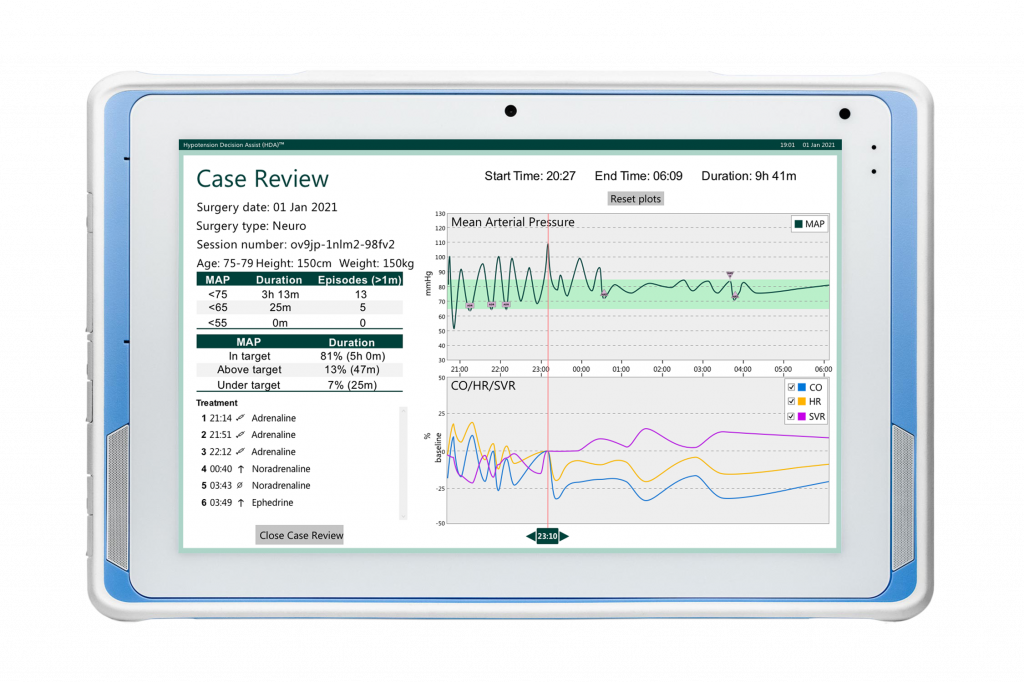
Hypotension Case Review – HCRTM
Hypotension Decision Assist – HDA™ has been designed for and with anesthesiologists, to assist anesthesia healthcare professionals to manage the blood pressure, hemodynamic stability and the cardiovascular system during surgery where an arterial line is present and arterial pressure is being continuously monitored. HDA™ provides an intuitive visualization via a single at-a-glance screen.
HDA™ key features
- Helps better assess and manage hypotension, adding value to existing patient monitoring
- Innovative visualizations in a highly intuitive user interface, with minimal training needed
- Connects digitally to the patient monitor through serial or network connections
- Easy out of the box installation, customer installable
- Streams the invasive arterial blood pressure (ABP) waveform through our patented algorithms providing:
- Trends in cardiac output (CO) and systemic vascular resistance (SVR)
- Cumulative time at different mean arterial pressure (MAP) thresholds, including hypotension
- Advanced signal quality analysis to ensure high quality, artefact free, data for patient care and data analytics
- Hypotension Case Review – HCR™ – end of surgery complete case review summary visualizes hypotensive episodes and parameters over the entire operation
- Network & Cloud connected – enables remote software upgrades and maintenance as well as access to Directed Systems’ secure DS Aware, which provides detailed case data storage, quality metrics and statistics.
Expected benefits of HDA™
- No costs of disposables or reusable sensors – on-going total cost of ownership low
- Help anesthesiologists to better manage blood pressure and the cardiovascular system including the detection and control of episodes IOH and cumulative IOH during surgery within user defined limits.
- Contribute to reducing hospital costs: an independent study by Keuffel et al (2019) showed that controlling IOH more effectively could save between $119-$458 per non-cardiac surgical patient1
currently only available in the USA
The Problem of Intra-operative Hypotension
Intra-operative hypotension (IOH) is a common and frequent occurrence in patients undergoing general anesthesia for non-cardiac surgery. A 2014 study of almost 17,000 anesthetic records revealed that 26% of the surgical patients involved had a peri-operative systolic blood pressure of <80mmHg for >5minutes2
IOH is associated with
Post-operative mortality3
Acute kidney injury (AKI)
Myocardial injury (MI)
Studies have shown that 30-day mortality was strongly related to time-weighted average intraoperative MAP4.
The threshold for myocardial injury is a MAP <65mmHg. The threshold for renal injury may be higher, possibly nearer 75mmHg. A few minutes of a MAP <55mmHg is associated with AKI and MI and have been demonstrated to increase markedly with prolonged intra-operative hypotension5.
“there does not appear to be any safe duration of a MAP less than 55 mmHg”
(Walsh, 2013)
Cumulative total time of IOH matters…
- MAP below 60–70 mmHg among adults is associated with increased risk of acute kidney injury (AKI), myocardial injury (MI), and mortality, and the risk is a function of both hypotension severity and duration6.
- Patients are at increased risk of AKI when their cumulative time below a MAP of 65 mmHg reaches or exceeds 13 minutes8
- When patients fall even further below this threshold (for example, MAP below 55 mmHg), even short durations are associated with increased risk of AKI7
download brochure
- Eric L. Keuffel, John Rizzo, Mitali Stevens, Candace Gunnarsson & Kamal Maheshwari (2019) Hospital costs associated with intraoperative hypotension among non-cardiac surgical patients in the US: a simulation model, Journal of Medical Economics, 22:7, 645-651.
- Nair et al., Anesthesia information management system-based near real-time decision support to manage intraoperative hypotension and hypertension. Anesth Analg 2014; 118: 206–214.
- Monk TG, Saini V, Weldon BC, Sigl JC. Anesthetic management and one-year mortality after noncardiac surgery. Anesth Analg 2005; 100: 4-10.
- Mascha EJ, Yang D, Weiss S, Sessler DI. Intraoperative Mean Arterial Pressure Variability and 30-day Mortality in Patients Having Noncardiac Surgery. Anesthesiol 2015; 123:79–91.
- Walsh M, Devereaux PJ, Garg AX, Kurz A, Turan A, Rodseth RN, Cywinski J, Thabane L, Sessler DI. Relationship between intraoperative mean arterial pressure and clinical outcomesafter noncardiac surgery: toward an empirical definition of hypotension. Anesthesiol 2013; 119: 507–515.
- Sessler, D. I., Bloomstone, J. A., Aronson, S., Berry, C., Gan, T. J., Kellum, J. A., Koepke, E. Perioperative Quality Initiative consensus statement on intraoperative blood pressure, risk and outcomes for elective surgery. British Journal of Anaesthesia, 2019; 122(5), 563–574.
- Salmasi, V., Maheshwari, K., Yang, D., Mascha, E. J., Singh, A., Sessler, D. I., & Kurz, A. Relationship between Intraoperative Hypotension, Defined by Either Reduction from Baseline or Absolute Thresholds, and Acute Kidney and Myocardial Injury after Noncardiac Surgery. Anesthesiology, 2017; 126(1), 47–65.
